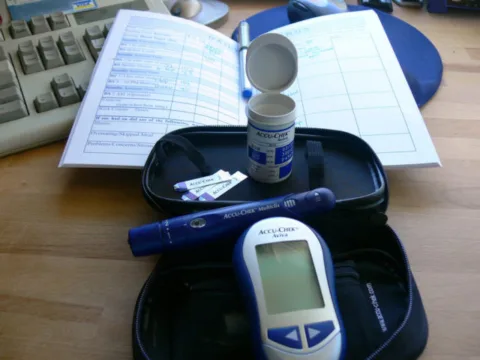
Being pregnant with gestational diabetes is not as easy as some people portray it to be.
When you’re diagnosed with gestational diabetes, you have to change the way you think, eat, and live.
You can’t just assume that this is a condition that will correct itself during the course of your pregnancy. And you certainly don’t want to ignore it because it can cause irreversible harm to you and your baby.
Some of the ways that you’ll have to change your lifestyle include:
- Counting carbohydrates
- Drinking more water
- Exercising more
- Testing blood sugars several times a day
- Paying close attention to how you feel
- Getting plenty of rest
This may seem like a very easy list of things to do. But when you’re pregnant and struggling with food aversions, cravings, bouts of physical discomfort, and/or raising other children, you’ll find that making those changes can be very challenging.
The Challenge of Counting Carbs
Counting carbs as part of the gestational diabetes diet plan seems easy when you have a dietitian in front of you. But when left to your own devices, it sometimes gets confusing.
For example:
- Before my diagnosis, on a good day I would normally have some fruit, eggs, and maybe a piece of toast and coffee.
- After my diagnosis, I found I could only eat 2 eggs and half a piece of toast if I wanted my numbers to stay within normal range.
Each person’s body responds to gestational diabetes differently. While many women are able to manage it with just diet and exercise alone, I was not so fortunate.
No matter how much I starved (monitored my carb intake) myself, I could not get my blood sugars in the normal range.
If you have trouble getting your numbers down to where they need to be — like I did — even though you’re doing everything that you’re supposed to, then you may need a little medical intervention to help. It’s not your fault. The culprit is the way your body processes foods when you’re pregnant.
Keeping Your Blood Sugar Levels In Check
According to my doctor, the suggested blood sugar levels for gestational diabetics are as follows:
- Fasting or before meals – 95 mg/dl or less
- 1 hour postprandial or 1 hour or less after meals – 140 mg/dl or less
- 2 hour postprandial or 2 hours or less after meals – 120 mg/dl
- Anything over 200 is dangerously too high
A good way to regulate blood sugar levels is to exercise every day. Even if all you can manage is a 15-minute walk, do it! The results start to show a few days later by giving you lower fasting numbers — which makes regulating your other numbers much easier.
However, you should avoid exercise if your blood sugar is over 200 mg/dl. At that point, exercise can cause the body to release toxins into your bloodstream and can cause your body to go into a state of ketosis — which could be harmful to both you and baby.
Gestational Diabetes Medications
It’s not the end of the world if you end up struggling while on the gestational diabetes diet.
There are medications you can take that make it easier for your body to do its job properly, while keeping you and your baby healthy.
Glyburide was initially prescribed for me. But every time I took it, it seemed to make my numbers spike. That is not a normal reaction and it apparently only happens in a small percentage of pregnancies. Needless to say, I was soon switched over to insulin.
Depending on how and when your blood sugar levels spike and respond during the day, you may end up taking medication or insulin several times a day.
Many women fear using insulin because there is a slight chance it could interfere with the normal process of their pancreas. But if you’re body doesn’t respond to medication like it should, then insulin is the next best — and safest — alternative.
Now these medications won’t make your gestational diabetes go away. But they will help keep your body from overloading your system with high levels of glucose — which can be toxic.
They can also help make you feel better and make it easier for you to continue the rest of your pregnancy as a gestational diabetic comfortably, so you can give your baby a better chance at life.